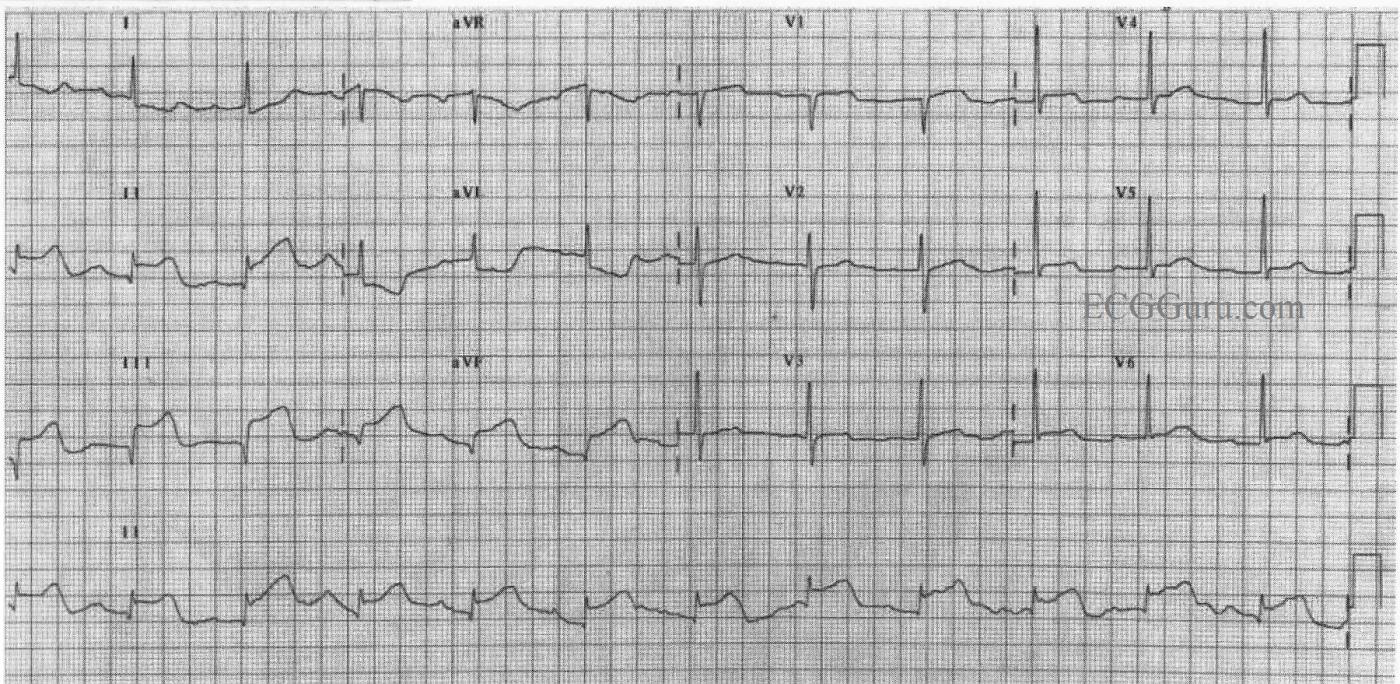
In this ECG, there is ST elevation in II, III, and aVF and reciprocal ST depression in I and aVL, indicating acute inferior wall M.I. Also, this patient has developed pathological Q waves in III and aVF, and probably II as well, indicating permanent damage to the myocardium. A ventriculogram or echocardiogram will confirm akinesis of the inferior wall in most cases. In this ECG, there is no ST depression in V1 through V3, so we can hope the posterior wall has been spared. Notice the flattening of the ST segments in the elevated leads. This is a sign of CAD. Last week's ECG had coved upward (frowning) ST segments, which are even more sinister looking. Lead V1 has the flattening, and a pathological Q wave. When V1 looks "sick" and V2 looks "well", there is a good probability of right ventricular injury as well. Lead III has a taller ST segment than Lead II. This has also been shown to be a marker of RVMI. Regardless, a right-sided ECG, or at least a V4 right, should be obtained in any IWMI, since the RCA often supplies both the right ventricle and the inferior wall of the left ventricle.
The rhythm in this ECG is interesting, as well. It appears to be sinus, but it is difficult to evaluate P waves. In the Lead II rhythm strip, they appear to change in morphology. Because the R to R interval remains constant, we feel this change in appearance is due to baseline artifact caused most likely by patient movement such as breathing. What do you think?
Our thanks to Andrew Porter for contributing this ECG.
All our content is FREE & COPYRIGHT FREE for non-commercial use
Please be courteous and leave any watermark or author attribution on content you reproduce.